 Last year I read Simon Borg-Olivier’s idea that the mysterious Pranayama practice of Plavini was essentially a form of lung packing (pushing extra air into the lungs to fill them beyond normal volume)and not the filling the stomach with air, as it often described.
Last year I read Simon Borg-Olivier’s idea that the mysterious Pranayama practice of Plavini was essentially a form of lung packing (pushing extra air into the lungs to fill them beyond normal volume)and not the filling the stomach with air, as it often described.
A couple of years ago I stopped packing and teaching packing to most students, feeling it to be unnecessary and probably not too good for the lungs. It also just didn’t seem like good yoga. Many also consider it to be a factor in many lung squeezes(lung oedema), which we’ll come to.
That said, Mr Borg-Olivier is one of the most experienced Yoga teachers around and a great free-diver, so I’m inclined to agree with him. It is listed as one of the 8 principle Pranyams though I have never heard of anyone teaching it or practising it. Except maybe Mr Borg-Olivier.
When packing, one fills the lungs and then gulps down extra air into the lungs. This stretches the membrane of the alveoli, allowing a person to expand their total lung volume, up to three litres in some cases.
Whether it is a Yogic practice or not, there seems to be relationship between lung packing and squeezes. Something which would seem to be counter intuitive, if packing means more air, one should be less likely to suffer lung squeeze, squeeze being caused by extreme negative pressure within the alveoli.
There are many people who deny a link, but they seem to generally be people who practice packing. Naturally they would have some resistance to the idea that it could induce squeezes.
For those who believe in a link, there have been various theories put forward. I won’t go into them here as I believe relatively recent research gives a better idea how packing could be a factor in squeezes.
For people who dislike scientific jargon I will summarise the research simply. Packing, when practised by trained divers, causes air to escape into the chest cavity. In trained free-divers this is normally asymptomatic, (there are no symptoms, no pain, no blood and no difficulty in breathing.) The alveoli are simply swollen with so much air that some escapes into the chest cavity. This was shown with CT scans to be the case, to varying degrees in all the free-divers trained in packing. (One didn’t have air in the chest cavity, but was later shown not be proficient in the technique.
This research now provides a more satisfactory reason why packing might be related to squeeze.
With packing you fill the lungs and overfill them, creating tiny tears in the lining. If you then dive to below residual volume, causing blood shift, you are creating the opposite effect in the alveoli. They compress and the capillaries around them swell with blood to fill the space.
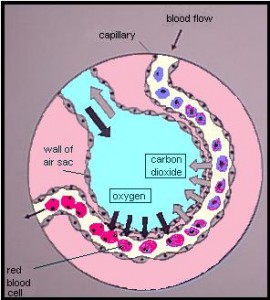
If the membrane between alveoli and capillary has been compromised before the dive by packing, then on the ascent to the surface it is easy to imagine that when the alveoli expand once again some of the blood may stay in the air space. This will compromise gas exchange and may lead to coughing of blood or plasma.
Lung squeeze is free-diving’s dirty little secret and it is much more common than people let on. See Sebastien Naslunds great article.
On many free-diving courses squeeze is but briefly mentioned and there is often no mention of a possible link between packing and squeeze, though often they are taught at the same level. The conclusion of this research is that the practice of packing is essentially a repeated barotrauma(pressure injury) and the accumulative effects are unknown. It therefore seems strange that packing should be thought at the intermediate, level as it is on many courses.
So now whether packing is really the mysterious Plavini pranyam or not seems immaterial. Unless you really into competition, packing seems like a needlessly risky activity, especially for ex-smokers or those whose lungs might not be as robust as they should be.
And besides Jaques Mayol did over 100 metres without packing, so what’s the need?
Here’s the abstract from the research so you can make up your own minds..
Abstract
Glossopharyngeal insufflation causes lung injury in trained breath-hold divers.
Source
Department of Thoracic Medicine, Concord Repatriation General Hospital, Concord, Sydney, New South Wales, Australia. stev78@optusnet.com.au
BACKGROUND AND OBJECTIVE:
Glossopharyngeal insufflation (GI) is a technique practised by competitive breath-hold divers to enhance their performance. Using the oropharyngeal musculature, air is pumped into the lungs to increase the lung volume above physiological TLC. Experienced breath-hold divers can increase their lung volumes by up to 3 L. Although the potential for lung injury is evident, there is limited information available. The aim of this study was to examine whether there is any evidence of lung injury following GI, independent of diving.
METHODS:
Six male, competitive breath-hold divers were studied. CT of the thorax was performed during breath-holding at supramaximal lung volumes following GI (CT(GI)), and subsequently at baseline TLC (CT(TLC)). CT scans were performed a minimum of 3 days apart. Images were analysed for evidence of pneumomediastinum or pneumothorax by investigators who were blinded to the procedure.
RESULTS:
None of the subjects showed symptoms or signs of pneumomediastinum. However, in five of six subjects a pneumomediastinum was detected during the CT(GI). In three subjects a pneumomediastinum was detected on the CT(GI), but had resolved by the time of the CT(TLC). In two subjects a pneumomediastinum was seen on both the CT(GI) and the CT(TLC), and these were larger on the day that a maximal GI manoeuvre had been performed. The single subject, in whom a pneumomediastinum was not detected, was demonstrated separately to not be proficient at GI.
CONCLUSIONS:
Barotrauma was observed in breath-hold divers who increased their lung volumes by GI. The long-term effects of this barotrauma are uncertain and longitudinal studies are required to assess cumulative lung damage.

Trackbacks/Pingbacks